May 9, 2021
Nursing students played a vital role in Israel’s fight against the global pandemic, with many recruited to bolster COVID wards at the height of the outbreak.
When a family friend of nursing student Yishai Cooperman asked him what his hospital could use in way of donations, Cooperman had a unique suggestion.
Rather than asking to put money toward more personal protective equipment (PPE) or ventilators, Cooperman asked for a guitar.
The simple string instrument was a surprising source of comfort at Jerusalem’s Shaare Zedek Medical Center during the past year.
“At the time, volunteers were banned because of COVID restrictions, so many of us attempted to bring some joy to patients in more untraditional ways,” he said. “For a patient, being in a COVID ward is lonely and a simple song would raise someone’s mood in such a dramatic way.”
Even doctors attempted to spread the cheer and the occasional strum of a guitar was one of the few signs of joy emanating from halls that have seen far too much sorrow.
Although Israel is now riding a wave of success from vaccines and many makeshift COVID-19 wards have begun to close, life was very different just a few months ago. Last January, the country hit its peak with nearly 8,500 new positive cases. To date, more than 6,300 Israelis have lost their lives to the disease.
The onset of COVID-19 shocked many, but for those in the midst of nursing training, nothing could adequately prepare them for how life changed during 2020. Ahead of International Nurses Day, marked on May 12, Israeli nursing students conveyed how this tumultuous year presented them with the greatest challenge of their lives.
“We had to adapt,” New Jersey immigrant and Jerusalem College of Technology nursing student Shoshanna Mayer said.
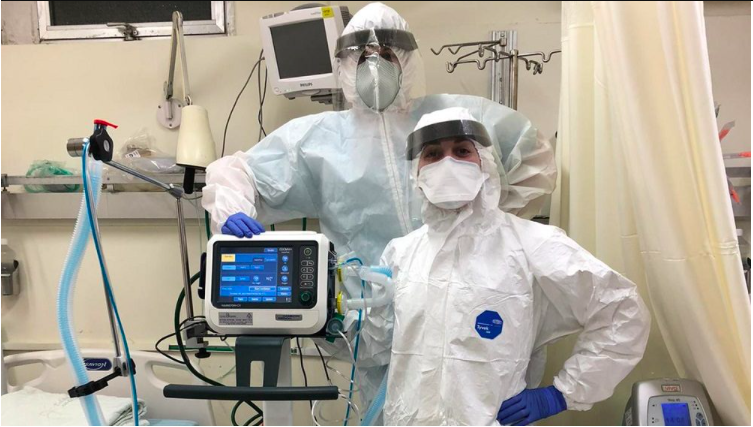
Mayer volunteers as an Emergency Room nurse in Hasharon Hospital at the Rabin Medical Center in Petach Tikva. During the pandemic, the relatively small suburban hospital was converted to a COVID-only facility. There, Mayer had to adhere to the strict regulations set by the Ministry of Health, wearing uncomfortable (but required) PPE for up to 11 hours a day while pregnant.
Mayer is one of many women nursing students at JCT who juggle being a working mother with a high-stress job.
“As a school with many religious students, it’s not uncommon to see a woman pursuing her nursing degree while also attending to up to 10 kids at home,” said Dr. Ahuva Spitz, head of JCT’s nursing program. “In many ways, though, their personal life allows them to bring a wealth of knowledge to the job.”
However, COVID-19 presented a unique set of challenges, especially since it’s not always obvious when someone is suffering from the virus.
“There was no set way of understanding who has COVID. There was something about this illness that it took a different course with each person,” Spitz explained.
Mayer saw this phenomenon firsthand. She remembers attending to a stroke victim with the minimal amount of PPE, never thinking that his symptoms were signs of COVID-19. After his rapid test came through with a positive result, Mayer felt uneasy being in such close proximity to an infected patient without wearing the proper gear.
“It’s very hard. As much as you try to prepare, you can get caught off guard. Older patients don’t know if they have a fever, for example, so you can’t go by just what they tell you in an interview,” she said.
The lack of manpower and strict protocols certainly took a toll, but Mayer was most impacted by how emotional her job became on a daily basis.
“A COVID patient can go down fast,” she said, explaining that nurses had to work quickly with minimal room for error.
She recalls one COVID-19 patient in the intensive care unit who was “in really bad shape. There was a man lying there, you can tell he used to be independent, but suddenly you can’t recognize the man he used to be anymore.”
The patient was fiddling with his phone, eager to read farewell messages coming in at a rapid pace from his loved ones. Mayer sat by his side and with her PPE-gloved hands, helping him go through the outpouring of love he was receiving in real-time. She also helped him make phone calls to his children who thought they may never see their father again.
“I had the mask and visor on, my vision was fogged up and I was terribly hot,” she said. “But I sat with him because I knew his family needed this right now. No training really prepares you for this.”
Despite this, JCT made it a priority to proactively prepare their students for the moment the pandemic hit.
“As soon as COVID began we prepared presentations right away to train students who were in their third or fourth year of studie, since the Ministry of Health notified us that they may be drafted to help with the shortage of nurses on hand in hospitals,” Spitz said.
But even the most well-trained and educated nurse can be moved by suddenly playing a critical role in a dying patient’s life. Cooperman recalled the time he saw a patient just moments away from death.
“Nobody was really around him. Doctors were busy attending to other patients. It was clear he wasn’t going to make it,” Cooperman said.
The third-year nursing student sat next to him and read Vidui, the Jewish prayer for those who are gravely ill. When Cooperman returned to work the following morning, he saw the man’s grieving family – the patient had died overnight – tearfully asking if someone read the prayer on his behalf. When Cooperman told them he did so, they were able to breathe a sigh of relief.
“It meant so much to them. I wasn’t sure if it would, they struck me as traditional and not particularly religious, but you could tell they were grateful that their father heard this important prayer,” he said.
Cooperman’s experience reflects how thanks to technology, nurses were doing far more than administering care in 2020. Many of them were the last face a patient saw before their demise.
“Hospitals went through a huge change last year. Many patients who normally would come in stayed away and the ones we did see were very sick,” he said. “It was scary at first, but you get used to everything.”
If there is a silver lining to COVID-19 for nursing students, it’s that they were able to get intensive, on-the-ground training they would not have been otherwise accessed.
“I learned a lot this year,” Cooperman said. “It wasn’t enough to be good at just one thing in 2020. In treating COVID patients, I learned to use all kinds of equipment that I didn’t know existed. Doctors would often ask me for help in a procedure when there weren’t enough nurses around, so I was able to get real, valuable experience that a student normally wouldn’t receive.”
Mayer’s experience this year reinforced why she pursued a career in nursing.
“I like helping people,” she said. “I like providing empathy and care to those who need it most, which is exactly what I did this past year.”
See full article: https://www.israelhayom.com/2021/05/09/for-israeli-nursing-students-covid-era-spells-multitude-of-tests/



